Eclampsia

Eclampsia is seizures (convulsions) in a pregnant woman. These seizures are not related to an existing brain condition. Causes Doctors do not know exactly what causes eclampsia. Factors that may play a role include: Blood vessel problems Brain and nervous system (neurological) factors Diet Genes Eclampsia follows a condition called preeclampsia. This is a serious […]
Disease Prevented by Vaccines
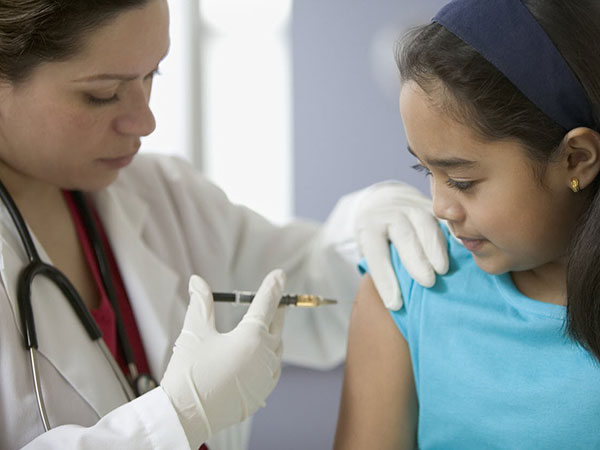
What are the vaccines a Bangladeshi kid receive? A Bangladeshi kid receives vaccines against 9 diseases: Tuberculosis, Polio, Diphtheria, Pertussis, Tetanus, Hepatitis B, Influenza type B infection, Measles and Rubella. Vaccine against Rubella is the latest vaccine added to schedule. Government of Bangladesh is now preparing launching of the 10th vaccine against Pneumococcus.
Anaemia During Pregnancy

What causes anemia during pregnancy? Your body uses iron to make hemoglobin, a protein in the red blood cells that carries oxygen to your tissues. During pregnancy, your blood volume expands to accommodate changes in your body and help your baby make his or her entire blood supply — doubling your need for iron. If […]
Breastfeeding

Advantage Of Breastfeeding Breastfeeding protects your baby from infections and diseases. Breastfeeding provides health benefits for mother. It’s free. It’s available whenever and wherever your baby needs a feed. It’s the right temperature. It can build a strong physical and emotional bond between mother and baby. It can give you a great sense of achievement. […]
Child Development Stage

Developement Stage of a Child Stage Motor Development 2 Months Smiles at the sound of your voice and follows you with their eyes around the room. 3 Months Raises head and chest when lying on stomach. Grasps objects. Smiles at other people. 4 Months Babbles, laughs, and tries to imitate sounds. Holds head steady. 6 […]
Common Complications of Pregnancy

What are some common complications of pregnancy? Some women experience health problems during pregnancy. These complications can involve the mother’s health, the fetus, or both. Even women who were healthy before getting pregnant can experience complications. These complications make the pregnancy a high-risk pregnancy. Getting early and regularprenatal care can help decrease the risk for […]
Common Signs of Pregnancy

What are some common signs of pregnancy? The primary sign of pregnancy is missing a menstrual period or two or more consecutive periods, but many women experience other symptoms of pregnancy before they notice a missed period. Missing a period does not always mean a woman is pregnant.Menstrual irregularities are common and can have a […]
